Dopamine does not cause pleasure; it causes "wanting" and is critical to addiction and social attachments
Key Takeaways
Dopamine does not cause pleasure. It causes “wanting” and craving.
The same dopamine pathways critical to addiction and are also critical to certain social attachments (monogamy and mother-infant bonding)
And our dopamine systems are highly influenced by genetics and environment; much of what we “want” may be outside conscious control.
Psychologists sometimes treat all kinds of loss in a similar way. Whether a loss of life, relationship, old habit, or personality trait, I’ve heard it conceptualized by therapists as grief.
Right before quarantine started, my ex informed me it was best if we didn’t talk anymore. For the first few weeks (maybe first few months…) of shelter-in-place, I remember really missing her, especially at night.
I also remember really missing the two cafes I frequented. Early mornings, evenings, and weekends, I’d go for a drink, and bring a book.
One type of missing made me feel ready to cry, the other not as much; but both shared a similar ache-y quality. Like my mind or body was reaching for something that could never be there.
I noticed quarantine give birth to some new habits too, some I didn’t like: a lot more Netflix binging, food binging. I felt especially drawn to these on the weekend. I tried a few times to stop. Again, it felt ache-y.
This led me down a research rabbit hole starting with the search terms “addiction,” “dopamine,” and “withdrawal.”
I still haven’t found direct evidence for dopamine’s role in grief, but I discovered some incredibly interesting research, seemingly related.
The below is an effort to distill the research. Much is included and cited. Key takeaways are at the top and section headers are bolded for easy skipping. If you’re interested in learning more, I’ve included citations, and the two main papers that guided most the research were “Is Social Attachment an Addictive Disorder?” and “The Debate Over Dopamine’s Role in Reward” (Insel 2003, Berridge 2007).
Teaser: A compulsion to act that escapes awareness
For five days a week, over six weeks, subjects sat in an empty room and read the following instructions:
To start the session press the left lever. During the session you are free to press the right lever as often as you like. Only presses on the right lever will have an effect; any responses on the left lever once the session has begun will have no effect. However you need not press either lever. When the red light comes on and stays on the nurse will give you an injection.
Depending on the week, subjects were given either placebo, 3.75mg, 7.5mg, 15mg, or 30mg of morphine (Lamb 1991).
During placebo week, subjects would stop pressing their levers by days four and five. For every morphine dose, however, lever pressing remained constant throughout the week.
At the end of each day subjects were asked “Do you feel the medicine?” and “Did you like the medicine?” Only the two highest morphine doses produced significantly more “yes” responses than placebo.
Morphine is quite addictive and the willingness to press a lever thousands more times for just 3.75mg of the drug speaks to this.
But subjects were unable to consciously differentiate between the feeling of low dose morphine and placebo. This speaks to something potentially haunting about the processes that underlie addiction: they may compel us to act differently, and we don’t even notice, or know why.
Quick overview on the dopamine system and addiction
The American Psychiatric Association classifies addiction as a severe form of “substance use disorder,” which is when “people keep using the substance even when they know it is causing or will cause problems” (APA). Put another way: “Addiction is a form of compulsive behavior with an increasing narrowing of the behavioral repertoire towards drug intake. The essence of addiction is a subjective sense of a loss of control” (Insel 2003).
The NIH and National Institute of Drug Abuse (NIDA) pour over $1.2 billion in research every year to understand and combat the epidemic of addiction. Although we lack great solutions, it is well understood that the brain’s dopamine and dopamine pathways are highly involved in the addiction process.
Most of the brain’s dopamine is released from a structure called the ventral tegmental area (VTA). It sits near the spinal cord and within the inner, older parts of the brain it sends projections to the amygdala (associated with threat processing), hippocampus (associated with memory formation), and nucleus accumbens (NAc, associated with initiating movement). This network within the inner limbic region of the brain is referred to as the mesolimbic dopamine pathway.
The VTA also sends projections to the newer prefrontal cortex (associated with executive and strategic thinking). This network is referred to as the mesocortical dopamine pathway.
Though the specific biological steps that lead to addiction are unknown, it is known that addictive drugs lead to high amounts of dopamine release within both these dopamine networks.
Dopamine was initially known for pleasure and reward
Dopamine was only discovered in 1957. Soon after, two studies solidified its initial reputation as the “pleasure chemical.” Dr. Robert Heath, a scientist with connections to MK-Ultra, implanted electrodes into the brain of “Subject B-19” (Heath 1972). When B-19 stimulated near his dopamine pathways, he expressed “feelings of pleasure, alertness, and warmth.” He also “had feelings of sexual arousal and described a compulsion to masturbate.”
A few years later Dr. Russel Portenoy ran a similar experiment with a female subject and observed similar results (Portenoy 1986). She stimulated so regularly at times, she ended up “neglecting personal hygiene and family commitments.” Heath and Portenoy concluded they discovered the “pleasure” centers of the human brain.
The belief that dopamine causes or somehow facilitates a sensation of pleasure remains quite pervasive. In 2014 headlines from a medical news site still read “Dopamine Is the Chemical That Mediates Pleasure in the Brain.”
However, starting in the late 90’s, Dr. Wolfram Schultz and Dr. Kent Berridge separately began compiling evidence that dopamine has very little to do with pleasure.
Berridge directly consulted Heath and Portenoy’s raw transcripts, and found that the supposed pleasure electrodes “did not cause much sensory pleasure after all”; and there was no “clear declaration of exquisite pleasure” (Berridge 2010, Berridge 2003). He also notes that although there was much talk of orgasm, it was never achieved via electrode stimulation.
Dopamine release is less about reward, more about cues and predictions

Dr. Schultz has been name-checked in quite a few bestsellers and podcasts including The Power of Habit, Hooked, and Atomic Habits. He has discovered a reliable and specific mathematical formula that can predict levels of dopamine release. His groundbreaking work has been used to explain how phones and apps keep our attention; and also how we might establish more positive behaviors and habits.
In his most cited study, he gave monkeys different quantities of juice and used electrodes to record dopamine activity (Schultz 1997). Trials began with displays of different colored shapes (each associated with different amounts of juice), then the monkeys were required to press a lever to receive their juice. At first, dopamine activity spiked immediately following the taste of juice. After more trials, greater amounts of dopamine released after the colored shape cue and less following the reward itself. Eventually nearly all the dopamine activity spiked after only the reward cue.
Schultz found that when a stimulus (such as the taste of juice, or color of a shape) causes dopamine release, it’s not because the stimulus itself was rewarding, but because the stimulus predicted reward. At first the monkey has not learned that the colored-shape predicts reward. Once the association is formed, the stimulus of the shape releases dopamine, rather than the reward. Hence the importance of cues in addictions and habits. *Note: His later experiments would reveal an important nuance to his mathematical model of dopamine release, which he calls “reward prediction error” (Schultz 2016). Not necessary to understand here, but useful to know
Schultz work fantastically, and with mathematical precision, shows what dopamine release “codes” for and how it’s related to reward prediction rather than the reward itself. But it provides slightly less insight into the subjective state a monkey or human might feel or perceive as a result of dopamine.
Dopamine causes “wanting” and craving, not “liking” or pleasure
“What originally attracted my colleagues and me to study dopamine… [were theories that] dopamine is an essential contributing cause of hedonic messages we experience as pleasure,” writes Berridge.
He continues: “But the data we collected soon forced a change of mind” (Berridge 2007)
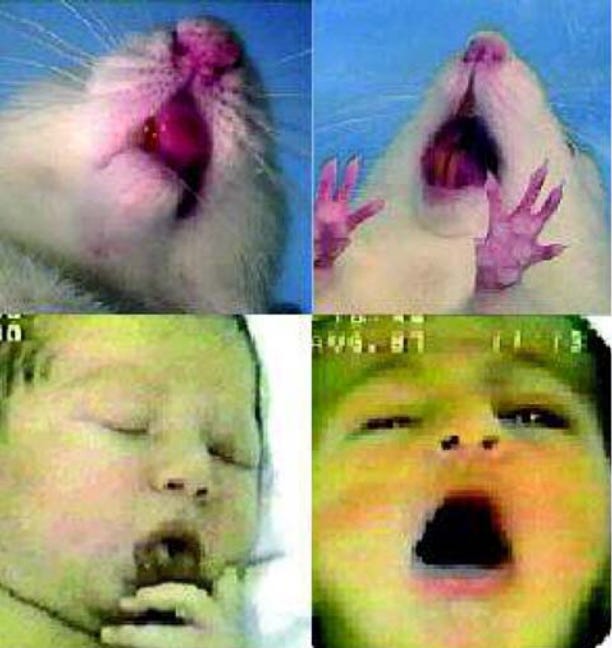
Many animals, including human babies, make similar facial expressions when they ‘like’ or ‘enjoy’ something versus dislike or are disgusted by something (see diagram). When animals like something their mouths tend to open wider and their tongues show slightly; when disliking or disgusted, they tend to wince.
To test whether dopamine caused or enhanced pleasure, Berridge and his colleagues used different chemical and surgical methods to remove and add dopamine to the brains of rats. In some, whole areas of the brain were removed; in others, chemicals were injected to either stimulate or block dopamine receptors. To be sure, he also genetically modified rats to either produce more or less dopamine. He then gave both the rats sugar pellets. Elevating or depleting dopamine did not alter the rats’ ‘liking’ reactions.
He also measured how willing the different rats were to press a lever for their sugar pellets. There were significant differences. Dopamine-elevated rats tripled their lever pressing activity, while dopamine-depleted rats would almost stop pressing at all.
-
Genetic and surgical modification of human subjects is not so simple. But Berridge cites a study on Parkinson’s patients, who experience a dramatic decay of dopamine neurons.
L-DOPA is a common treatment and is the closest chemical to dopamine that can be orally ingested and make it to the brain. Dr. Evans and his team gave Parkinson’s patients different amounts of L-DOPA, imaged their brains, and asked,
On a scale of 1-100 “Do you like the effects your feeling right now?” There was no relationship between score and dosage (Evans 2006).
He then asked, on a scale of 1-100, “Do you want more of what you consumed, right now?” A statistically significant difference emerged. Greater doses of L-DOPA were associated with a higher rating of “wanting more” and also more brain activity in dopaminergic regions.
With converging evidence in both animal and human studies, Dr. Berridge concluded that dopamine causes “wanting” but not pleasure or “liking.”
-
Berridge calls special attention to his use of quotation marks around both “wanting” and “liking.” They demarcate the non-conscious processes underlying “wanting” and “liking” that are “distinguishable from their subjective feelings.”
For instance, “liking” facial reactions to sugar are relatively automatic and separate from conscious awareness or the subjective feelings of pleasure of babies or animals. And dopamine induced “wanting,” measured by a rat’s increased willingness to press a lever for sugar and a human’s willingness to press a lever for 3.75mg of morphine, is also automatic and not necessarily conscious. Both can operate beneath our awareness.
Dopamine induced “wanting” can compel an organism to act.
*An interesting note on L-DOPA: Eventually, some Parkinson’s patients treated with L-DOPA develop a second disorder, DDS, Dopamine Dysregulation Syndrome, where dopamine levels become hyper-elevated and symptoms include compulsive behaviors such as OCD and gambling.
Dopamine causes mother-infant attachment
Addiction is a brain disorder characterized by pathological “wanting.” It is an obsession that compels us toward some stimulus even if harm and risk stand in the way. It causes injury and death for many. But maybe some addictions, or addiction-like behaviors, help us thrive and survive.
In his review “Is Social Attachment an Addictive Disorder” Dr. Thomas Insel provides evidence of the remarkable similarities in the biology of addiction and certain social attachments (Insel 2003).
When a rat mother is given the choice between access to cocaine or her newborn pups, she prefers her pups (Mattson 2001). After the pups turn 16 days old, she reverses and chooses the cocaine.
To test whether this mother-infant attachment was due to the same dopaminergic system implicated in substance abuse, researchers tested two alternative scenarios: first, they surgically removed parts of the dopaminergic pathway and, second, they used chemicals (including cocaine) to block normal dopamine signaling in that pathway.
Both experimental conditions of reduced dopamine activity significantly reduced the rat mother’s approach behavior to her new pups.
For certain periods of time, a rat mother may find her pups more dopaminergically stimulating than cocaine. And to a significant extent, her attachment is mediated by the same dopaminergic pathways implicated in drug abuse.
Dopamine causes certain male-female attachment
The Prairie vole and Montane vole species are virtually identical except for one important trait: Prairie voles are monogamous and Montane voles are polygamous. A small genetic difference causes female Prairie voles to have more oxytocin receptors and male Prairie voles to have more vasopressin (the male version of oxytocin) receptors in their dopamine pathways (Insel 1998). Importantly, oxytocin and vasopressin tend to be released during affiliative social behaviors, such as sex.
Insel and his colleagues were able to show that by experimentally altering dopamine activity, they could change whether prairie voles were monogamous or polygamous.
First, they tested dopamine receptors directly. They were able to induce pair-bonding in Prairie voles in the absence of mating by stimulating a specific kind of dopamine receptor in the nucleus accumbens (Wang 1999). By blocking the same receptors, they blocked pair-bonding during mating.
Next, they altered dopamine pathway activity by way of oxytocin and vasopressin manipulation. In a similar fashion, they were able to induce and block pair-bonding by injecting oxytocin and oxytocin antagonists, respectively, into the dopamine pathways of female prairie voles (Insel 1995). They replicated this in male prairie voles using vasopressin and vasopressin antagonists (Lim 2002).
As with mother-infant attachment, the same dopamine pathway implicated in addiction disorders, mediates male-female attachment as well, at least for mice and voles.
-
Insel explains the most likely reason addiction and attachment share biological pathways and genes is that “these pathways and genes evolved not for drug abuse but for mediating the motivational aspects of social interaction.” Drugs hijack a natural process that normally serves an evolutionary purpose.
He hypothesizes that drug use sometimes “serves as a substitute for social attachments and that a common neurobiology underlies the major forms of attachment.”
Dopamine functionality and our attachments are sometimes beyond our control: genetics and environment
Due to a combination of genetics and environment, addiction is highly heritable. In identical-twin studies, substance-abuse disorders show a 0.7 factor of heritability (Ducci 2012). And if addiction occurs at least once in a household, it is much more likely to occur again. Specific genetic markers are also being correlated with addiction (Karamitros 2018).
As discussed earlier, predisposition to certain social attachments have clear genetic components too. A similar gene to the AVPR1 vasopressin gene found in prairie voles has been found in humans. Human males with the monogamous-vole variant have slightly more stable relationships through life (Walum 2008).
Attraction to certain social attachment styles is also influenced by early gene-environment interactions. At least with rats, depending on the mothering styles, genes will turn on or off resulting in different levels of production and sensitivity to stress hormones. Baby rats can also learn to become attracted to stimulus that normally induces stress and aversion in normal rats. Professor Robert Sapolsky titled a paper on these effects “Any Kind of Mother in a Storm” (Sapolsky 2009).
It seems much of what we want may be biologically shaped by things outside our control.
The “Dark Side of Addiction”: stress pushes us further toward a substance
The closest line of research I found toward understanding dopamine’s role in grief comes from Dr. George Koob, who publishes continuously on “The Dark Side of Addiction” (Koob 2018).
The Dark Side of Addiction, which Koob also calls the “anti-reward system,” is the strong negative reinforcing effects of addiction.
You are willing to work just as hard to get more of the positive effects of a drug or stimulus (positive reinforcement), as you are to remove the strong painful after-effects of stress and withdrawal-like symptoms (negative reinforcement).
Koob believes a few key chemicals mediate the stress and pain of withdrawal symptoms, specifically corticotropin-releasing factor (CRF) and dynorphin. In rat studies, blocking CRF and dynorphin reduces withdrawal-like symptoms (e.g. anxiety and paw tremors) (Zorrilla 2014).
These chemicals are supposedly normally released after dopamine release to keep the body in homeostasis. But when released in high amounts, as might happen after a drug binge, they lead to withdrawal and withdrawal-like symptoms. And this cycle perpetuates binge-withdrawal, driving toward stronger addiction.
Conclusion
Whether or not the evidence for dopamine’s critical role is overturned by future research, a tremendous amount of human energy is directed toward objects of our “wanting” and craving. And much of what we want and how it influences us may be determined unconsciously by genetics or environment.
The evidence supports dopamine’s role in at least the “wanting” and craving of addictive drugs, mother-infant attachment, male-female pair bonding, and normal pleasurable rewards such as juice and sugar. It seems likely that all other conscious and unconscious wanting is also caused by dopamine. So how much of our actions have we chosen, rather than some combination of gene, environment, and dopamine systems has chosen for us?
Even something seemingly as significant as love or choosing a romantic partner, how much choice do we really have? From spending the last few years living in New York, I’ve noticed that I’ve begun to feel more physically attracted to a certain look and fashion. I don’t think I chose it; I was just surrounded by it.
Every city, family, and culture also has its own moral standards and status symbols; but also preferred colors, shapes, and sounds. What other choices am I not making? What else has dopamine compelled me to do?